Author: John Wilding
The clinical challenge
Glucocorticoids, which include long-acting corticosteroid preparations such as prednisolone and dexamethasone, are frequently used to treat inflammatory conditions such as asthma and exacerbations of chronic obstructive pulmonary disease, and other conditions including many autoimmune diseases, and also to reduce cerebral edema in association with brain tumors. More recently, the RECOVERY trial demonstrated their benefits in the treatment of hospitalized patients with severe COVID-19 infection, leading to widespread use in people with COVID-19. Hyperglycemia is a common adverse effect of high-dose corticosteroids, and can manifest as worsening glucose control in people with known diabetes and development of hyperglycemia in those without a history of diabetes.
The mechanisms by which corticosteroids cause hyperglycemia are complex, and include increased insulin resistance and impairment of insulin synthesis. Specifically, increased hepatic gluconeogenesis and increases in central and visceral adiposity, combined with greater lipolysis in peripheral fat stores and a rise in glucagon, all contribute to insulin resistance, while beta-cell function is reduced due to both direct effects and a reduction in the incretin effect. These processes can trigger hyperglycemia in those without diabetes, which is most common in people with pre-existing obesity and insulin resistance, and lead to a significant deterioration in glucose control in those with both type 1 and type 2 diabetes.
In a recent observational study from a UK hospital including 605 patients with COVID-19 pneumonia treated with dexamethasone (6 mg/day for 10 days as per the RECOVERY trial protocol), 11% of patients without diabetes developed hyperglycemia, and 70% of those with known diabetes (nearly a quarter of the cohort) experienced worsening of glucose control. Although it is possible that COVID infection itself might precipitate hyperglycemia, this is also true for other medical conditions that are treated with corticosteroids; hence the experience in the context of COVID seems relevant to other conditions.
A pragmatic approach to diagnosis and management
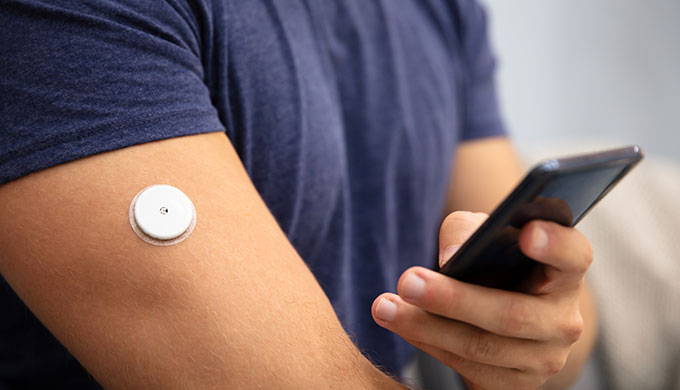
It is therefore essential to monitor glucose in all people being treated with high-dose corticosteroids – in the hospital setting this would usually require pre-meal testing and a test before bedtime (four tests per day). If hyperglycemia (defined as a capillary blood glucose above 11.1 mmol/L) develops for people with pre-existing diabetes, most guidelines advise increases in insulin doses for those already on insulin (a 20% increase in basal insulin dose is commonly advised as a starting point), and commencement of basal insulin (Neutral Protamine Hagedorn [NPH], at a starting dose of 0.3 units/kg per day) for those not taking insulin. Likewise, short-term use of basal NPH insulin may be needed in those without pre-existing diabetes. There is much less evidence for use of other glucose-lowering agents; although sulfonylureas and metformin are often used, they may not be sufficient to control hyperglycemia in many patients.
Finally, it is important to remember that follow-up of these patients is needed, and for those who require long-term steroid use, hyperglycemia can become chronic and may require ongoing treatment.
About the author

John Wilding
John Wilding, DM FRCP, leads Clinical Research into Obesity, Diabetes and Endocrinology at the University of Liverpool, UK.